Week 1 HW: Principles and Practices

Important: I use ChatGPT and Gemini to help me organize my ideas, translate some concepts and reunite everything!!
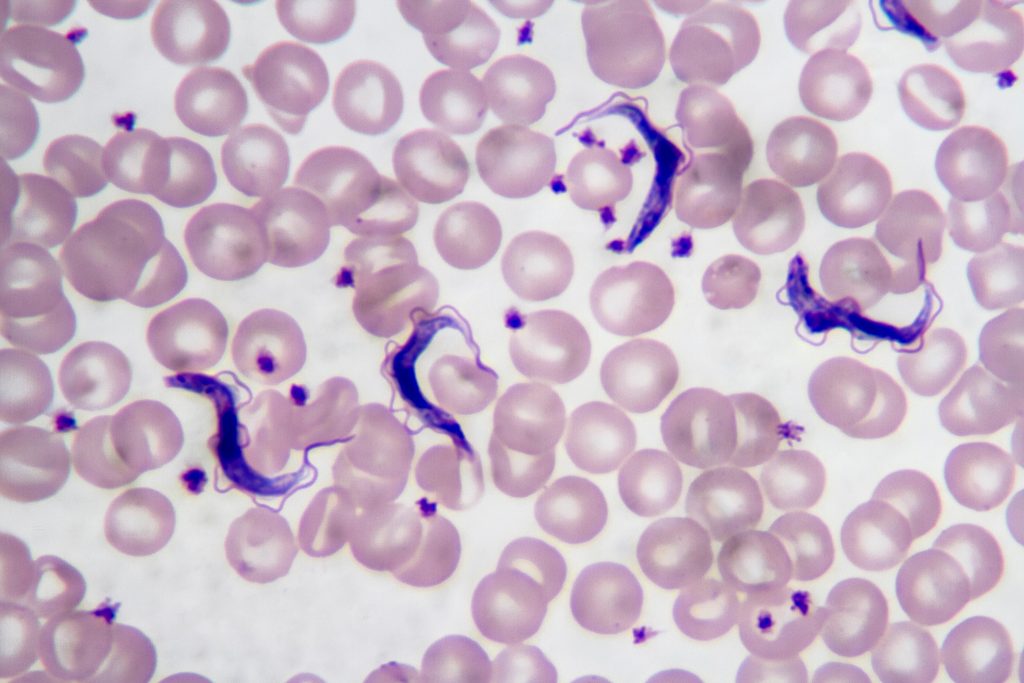
Chagas disease is a major public health problem in Latin America, especially in underserved regions. In Argentina, this disease mainly affects the northern part of the country, where high temperatures, rural housing conditions, poverty and limited access to healthcare favor the presence and spread of the insect vector vinchuca or “kissing bug” (scientifically called Triatoma Infestans). Many people living in these areas are diagnosed late or not diagnosed at all.
Early diagnosis is extremely important, since treatment is much more effective in the early stages of infection. However, current diagnostic methods often require multiple tests, specialized equipment, and trained personnel, which are not available at all in low-resource settings. In addition to this, several provinces such as Santiago del Estero, Formosa, Chaco, Tucuman and Jujuy include regions that are extremely difficult to access. Areas like El Impenetrable in Chaco or the rural forested regions are home of communities that lack basic services such as water, electricity and reliable transportation. These create favorable conditions for the presence and reproduction of vinchucas.
Given this, I propose the development of a nanobiosensor for the early diagnosis of Trypanosoma cruzi infection. The idea is to create a portable, low-cost diagnostic tool that could detect parasite-specific biomarkers such as Tc24 and SAPA proteins in simple biological samples like blood, allowing the fast and early diagnosis outside of centralized laboratories.
Governance/Policy goals
The main governance goal of this project is to ensure that the nanobiosensor is developed and used in a safe, ethical and socially responsible way, and it’s accessible to everyone, in order to maximize its public health benefits and minimizing potential harms.
Prevent harm and ensure safe use (non-malfeasance): this technology should not cause any harm due to inaccurate results, misuse, or unsafe handling. It should be easy to use, handled by a primary care doctor.Promote equity and fair access: this nanobiosensor should be accessible to everyone, especially to those most affected rural communities. The goal is the implementation of “Open Science” licensing for sensor’s design to allow local manufacturing in Argentina, reducing dependency on expensive imports, to avoid creating a technology that only benefits massive healthcare systems.Build trust and responsible data use: people must trust the diagnostic tool and the institutions using it. This includes clear communication, informed consent, responsible use of data, and education in healthcare systems and machinery.
Potential Governance Actions
a. Field-based validation and approval for point-of-care diagnostics
Purpose: nowadays, the diagnosis of Trypanosoma cruzi infection relies mainly on laboratory-based methods such as ELISA and PCR, which require specialized infrastructure and trained personnel, limiting their use in rural and low-resource endemic areas. At the same time, recent studies have explored biosensor-based diagnostics for other parasitic diseases, including malaria and leishmaniasis, demonstrating the potential of nanobiosensors for rapid and point-of-care detection. However, similar technologies for Chagas disease remain underdeveloped and poorly implemented.Design: this biosensor would be tested in real environmental conditions (high temperature, limited infrastructure, low-income facilities) in collaboration with local primary care centers and rural doctors. National health authorities (ANMAT) would review the results before approving large-scale use.Assumptions: it is expected that the validation and approval would be fast and without obstacles. We could also assume that communities and healthcare professionals will easily adopt this technology but we have to think about a potential resistance from large pharmaceutical companies or major laboratories that may see their market threatened.Risks of failure and success:- Risks of failure: if major corporations oppose the technology, it could lead to delays in approval and, consequently, limited availability. This sensor could also not be well-received due to a lack of local infrastructure or training.
- Risks of success: If the sensor is successfully adopted, it could create a demand that outpaces local production capacity, potentially causing shortages or uneven distribution.
b. Incentives for affordable and open-access design
Purpose: to reduce inequality in access, this action focuses on keeping the technology affordable and widely available.Design: public funding or academic grants could require that the nanobiosensor design be shared under open or non-exclusive licenses. Partnerships with public institutions, important researchers and local manufacturers could help reduce costs and support regional production.Assumptions: this assumes that researchers and developers are willing to share designs, data and manufacturing processes under open or non-exclusive licenses. It also assumes that open access or publicly funded models can remain economically sustainable while maintaining quality standards.Risks of failure and success:- Risks of failure: if public funding is insufficient or inconsistent, production quality could decline, resulting in unreliable diagnostic devices. Private companies may also be discouraged from participating due to limited commercial incentives.
- Risks of success: if open-access designs are widely adopted, a lack of clear coordination and quality control could lead to fragmented manufacturing, variable device performance or misuse.
c. Training healthcare workers and engaging communities
Purpose: a diagnostic tool is only useful if used correctly and understood by both patients and healthcare workers.Design: basic training programs would be implemented for healthcare workers on how to use the sensor, interpret results and explain them to patients. Community education could help reduce fear, stigma or misinformation related to Chagas disease, and also help prevent the infections.Assumptions: this assumes that training programs can be effectively delivered, that healthcare workers have sufficient time and institutional support to participate and that communities are open to engaging with new diagnostic technologies and to receiving education.Risks of failure and success:- Risks of failure: without adequate training or follow-up, healthcare workers may misinterpret results or use this tool incorrectly, leading to inaccurate diagnoses or loss of trust.
- Risks of success: if training and community engagement are highly effective, diagnosis rates may increase rapidly. This could potentially overwhelm healthcare systems that are not fully prepared to provide treatment, monitoring, or long-term care.
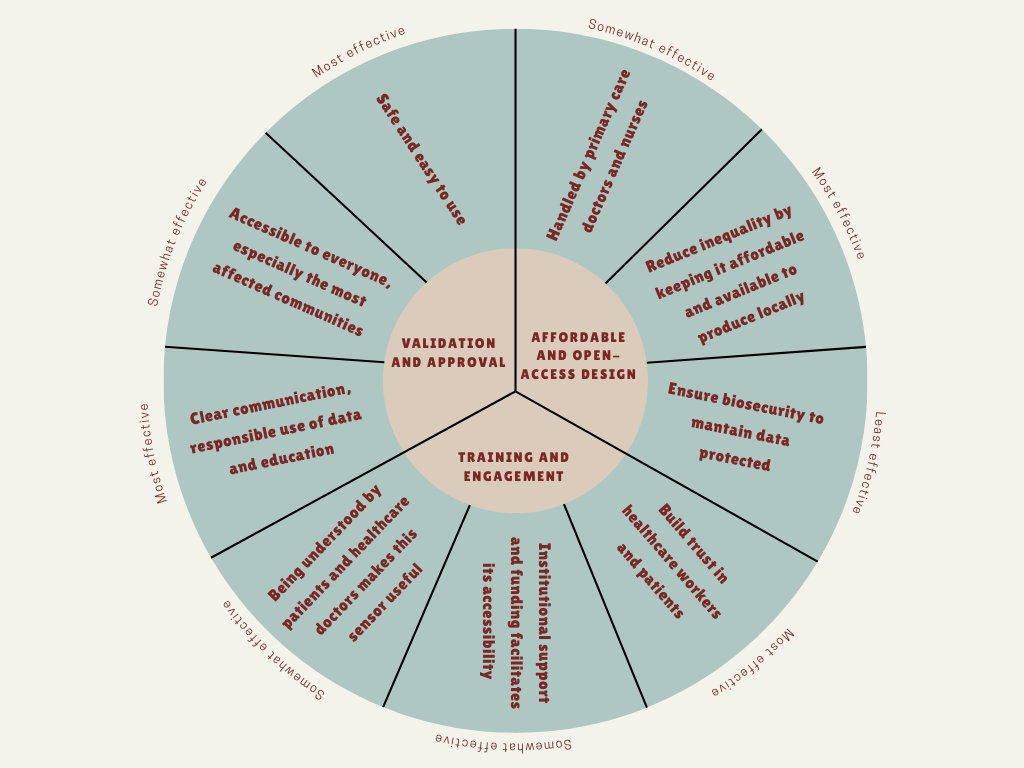

Based on the previous analysis, I would recommend a combination of Field validation and approval and Incentives for local manufacturing. I strongly believe that these actions are not sufficient on their own. For example, sharing the sensor’s “blueprints” ensures this technology is accessible and easy to develop, but it does not guarantee the quality control that only formal regulation can provide. Consequently, I propose that ANMAT as a regulatory agency and the Ministry of Health of Argentina should provide funding and legal approval exclusively to projects that commit to manufacturing this nanobiosensors, and keeping prices accessible not only for the public health system, but also for researchers and scientific institutes.
What we win and what we risk:
- To make the sensor low-cost and locally made, we must take on more responsibility in supervising the process. We will be choosing the “harder” path of managing our own production instead of the “easier” but more expensive path of importing finished technology from abroad. It’s the only way to become independent.
- Adjusting and testing the devices in the extreme conditions where most of the damned patients live will delay the official launch. However, this is a necessary sacrifice. Otherwise, we risk the sensors failing due to environmental conditions, leading to false negatives and destroying the community’s trust in the program.
Assumptions and Uncertainties:
- Political will: this plan assumes that the National Health System will keep Chagas disease as a priority and will not cut the budget needed for its treatment.
- Pathogen evolution: it is well known that pathogens tend to mutate in order to adapt and survive new environmental conditions, so it is uncertain if the protein used in this sensor will continue to function in a future. This is why this device will need periodic updates, as well as the studies on T. cruzi.
- Digital infrastructure: we assume that, even in remote areas, there will be a basic way to perform this analysis and measurements, and there will always be a healthcare worker around to do it.